Snoring, Sinus & ENT Specialist
- Dr Kenny Peter Pang
- Ear, Nose & Throat Consultant
- Otorhinolaryngologist
- MBBS MRCS(Edinburgh)(UK)
- FRCS(Edinburgh)(UK)
- FRCS(Ireland)(OTO)
- Masters Medicine (ORL)
- Founder, ASEAN Sleep Surgical Society
- Founding Member, International Surgical Sleep Society
- Member, American Academy Sleep Medicine
- Member, Singapore Sleep Society
- Member, World Sleep Society
- Board Member, Italian Sleep Disorders Board
- Member, British Association of Sleep Surgeons
- Member, European Academy of Sleep Medicine
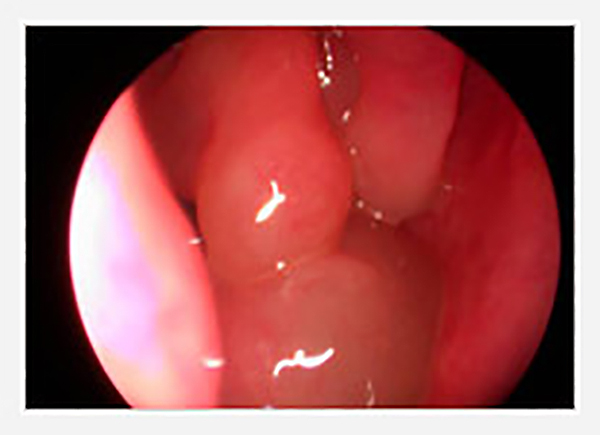
The pathogenesis of nasal polyposis is unknown
Polyp development has been linked to chronic inflammation and genetic predisposition. Most theories consider polyps to be the ultimate manifestation of chronic inflammation; therefore, conditions leading to chronic inflammation in the nasal cavity can lead to nasal polyps. Associated conditions include:
- Asthma (20-50% of patients with polyps),
- Allergic Rhinitis,
- Allergic Fungal Sinusitis (AFS) (polyps found in 85% of patients with AFS),
- Chronic Rhinosinusitis,
- Aspirin intolerance (8-26% of patients with polyps), and
- Alcohol intolerance (50% of patients with nasal polyps).
Several theories have been postulated to explain the pathogenesis of nasal polyps, although none seems to account fully for all the known facts. Some researchers believe that polyps are an exvagination of the normal nasal or sinus mucosa that fills with edematous stroma; others believe polyps are a distinct entity arising from the mucosa.
Patients with massive nasal polyposis typically present with
- severe nasal congestion (bad nose block),
- hyposmia to anosmia (no smell),
- lack of sense of taste,
- persistent back of nose flow,
- headaches, facial pain and discomfort are not uncommon and are found in the periorbital and maxillary regions.
Patients with solitary polyps frequently present with only symptoms of
- nose block, which may change with a shift in position
(i.e. while lying supine, the polyp may swing backwards, opening up the nasal cavity and in an upright position, the polyp has a more obstructive effect).
A Flexible Nasal Endoscopy is the best method to examine the nasal cavity and nasopharynx to fully assess the nasal anatomy and to determine the extent and location of nasal polyps. The anterior and posterior nasal space is examined carefully for other pre-existing disorders. Occasionally, mucus and pus due to sinusitis, arising from the middle meatus or the superior meatus would be visualized on endoscopic nasal examination. Nasal polyposis is a clinical diagnosis based on history and physical examination.
In general, imaging studies might be required. CT (computer tomography) scan of the sinuses can be very helpful. Coronal sinus CT is the imaging study of choice in the evaluation of patients with nasal polyposis. The CT scan is done to delineate sinus anatomy, disease extent and anatomical variants/bony landmarks.
Treatment
The management of nasal polyps should be based on the causative factors. Unfortunately, most cases of nasal polyps have an unknown cause.
- Even if the patient is allergic, it is controversial as to whether the management of his/her allergies would reduce or eliminate the polyps; hence, medications would be mainly symptomatic and supportive.
- Oral corticosteroids are the most effective medication for the short-term treatment of nasal polyps, and oral corticosteroids have been shown to be effective in shrinking the polyps. Unfortunately, oral systemic steroids have serious side effects if given at high doses and for long duration.
- Intranasal steroid sprays may reduce or retard the growth of small nasal polyps, but they are relatively ineffective in massive nasal polyposis.
- Endoscopic sinus surgery is the procedure of choice. With the advent of endoscopic sinus surgery, surgical treatment for sinus diseases has become safer, and the outcome has improved. With appropriate preoperative evaluation and planning, endoscopic sinus surgery is usually carried out in an ambulatory setting with minimal discomfort to patients. Patients with complicated sinus disease can also be safely treated with the new image guided systems which provide real time anatomical accuracy up to 1mm.
Definitions:
Asthma - is a chronic inflammatory disorder of the airways characterized by an obstruction of airflow, which may be completely or partially reversed with or without specific therapy.
Allergic Fungal Sinusitis – is now believed to be an allergic reaction to environmental fungi that is finely dispersed into the air. This condition usually occurs in patients with an immunocompetent host (possessing the ability to mount a normal immune response). Patients diagnosed with AFS have a history of allergic rhinitis.
Endoscopic Sinus Surgery – is a minimally invasive technique in which sinus air cells and sinus ostia are opened under direct visualization. This is done usually under general anaesthesia and with fibreoptic endoscopes through the nostrils of the patient.






